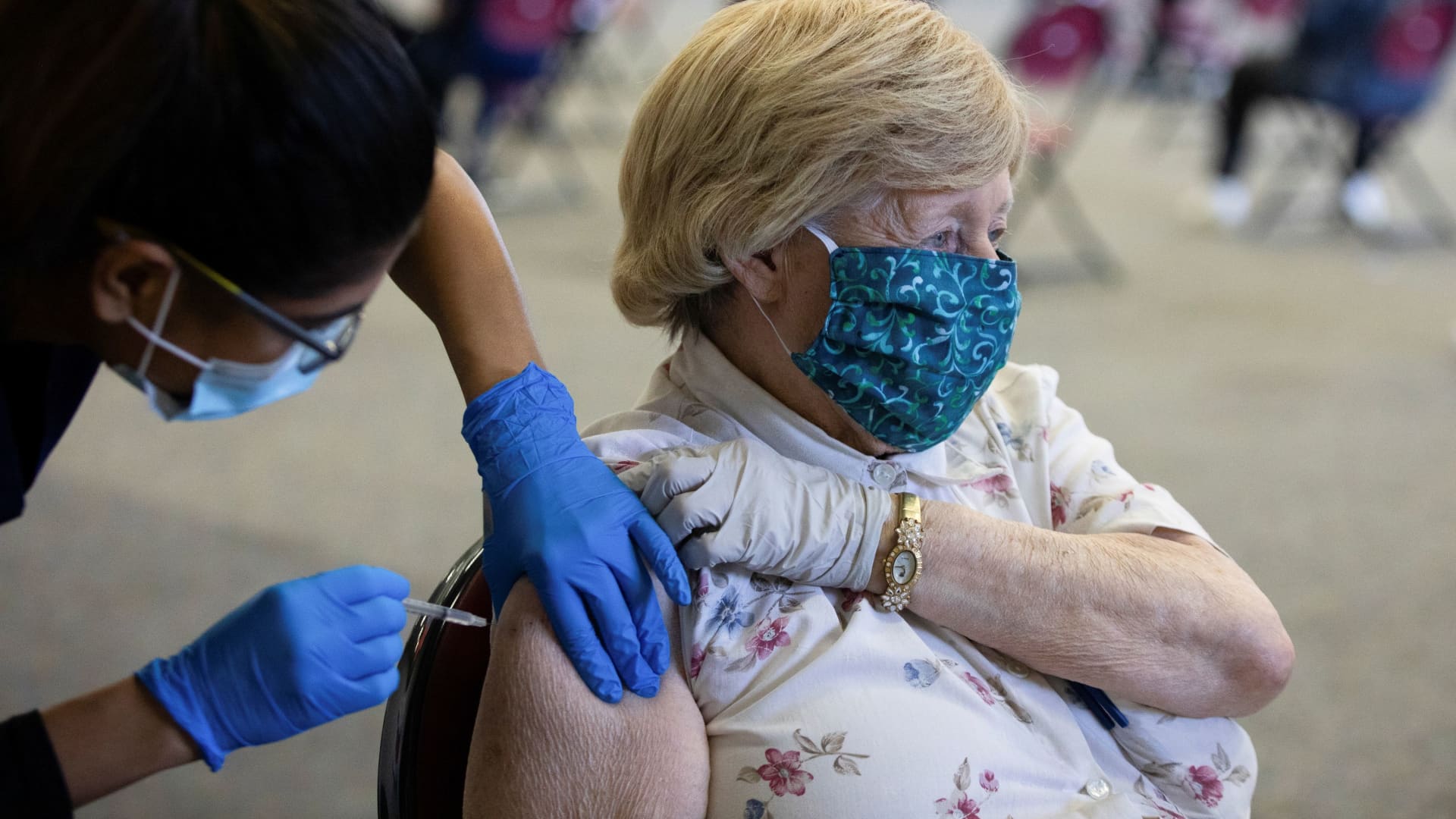
Covid vaccines prevented at least 330,000 deaths and nearly 700,000 hospitalizations among adult Medicare beneficiaries in 2021, the Department of Health and Human Services said in a new report released Friday.
Reducing hospitalizations due to vaccination has saved more than $16 billion in medical costs, according to the HHS report. According to the study, a 10% increase in immunization coverage was associated with a 12% and 15% decrease in the likelihood of hospitalization and death in adult Medicare recipients, respectively.
The HHS study examined county-level data on immunization rates and changes in hospitalizations and deaths in a sample of Medicare beneficiaries ages 18 and older. Texas and Hawaii were not included in the study due to incomplete vaccination data.
The overwhelming majority of Medicare beneficiaries, 86%, are 65 years and older. Select groups under the age of 65, such as people with disabilities, are also eligible. People who are not seniors make up about 14% of Medicare beneficiaries, according to data from the Centers for Medicare and Medicaid Services.
Older people are at highest risk of serious illness and death from Covid. Almost 93% of people age 65 and older in the US have received two doses of a Covid vaccine, according to the Centers for Disease Control and Prevention.
Despite immunization coverage within the highest-risk group, CDC data still shows an average of more than 300 people dying each day from Covid, while more than 3,300 are hospitalized each day. dr Ashish Jha, who heads the White House Covid task force, said 70% of Covid deaths occur in people aged 75 and older.
“This is unacceptable, especially because we can now prevent almost every Covid death in the country with vaccines and treatments that we have,” Jha told reporters during a call on Friday.
Although most people aged 75 and over have received their primary vaccination course, those who die are either not up to date on their booster shots or are not receiving treatments like Paxlovid if they have a breakthrough infection, Jha said. He added that death rates are dramatically higher in people in this age group who didn’t get their first booster shot last fall.
“If you are up to date with your vaccines and treated if you have a breakthrough infection, your chances of dying are close to zero even in this high-risk population,” Jha said.
Jha said the most important step people in this age group can take to protect themselves is to get the new booster shots, which target the dominant subvariant Omicron BA.5 along with the original Covid strain.
The original Covid vaccines were developed against the first strain that emerged in China in 2019, and their effectiveness in preventing infection and mild illness has decreased significantly as the virus has mutated. While they generally still protect against the worst of outcomes, their ability to prevent hospitalization has also declined over time, especially among older people who have not kept up with their vaccinations.
Health officials believe the new boosters will offer significantly better protection against disease now that vaccinations are in line with the main variant of Covid circulating in the US
But the FDA and CDC approved the new BA.5 boosters without data from human trials, so it’s unclear how much more effective they’ll be than the old shots. FDA officials said they approved the boosters using the same process they use every year to rotate flu vaccines, which is also not usually based on direct human data.
The HHS study did not look at the effect of booster shots on serious illness and death because these shots were not introduced until late 2021.
The FDA approved the Pfizer and Moderna vaccines in December 2020. Seniors were the first to receive the vaccines, and eligibility was gradually expanded throughout 2021.